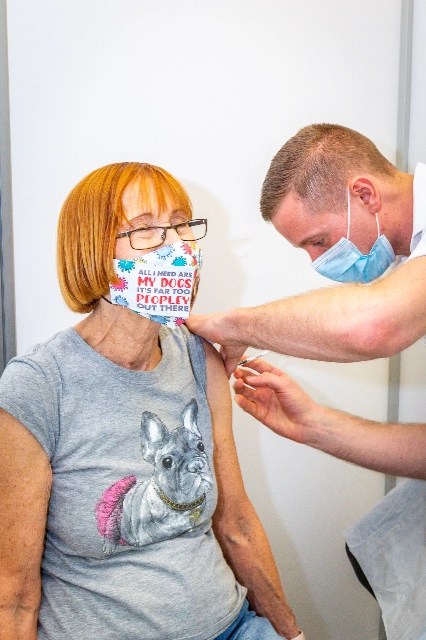
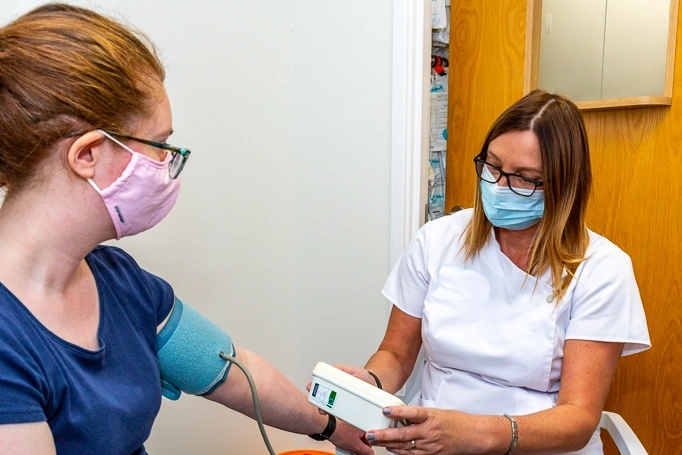
Advanced Services
Published on: 10th July 2013 | Updated on: 19th February 2024
There are currently nine Advanced Services within the NHS Community Pharmacy Contractual Framework (CPCF).
Community pharmacies can choose to provide any of these services as long as they meet the requirements set out in the Secretary of State Directions.
Other pages in this section
Other relevant pages and resources
National services provided by community pharmacies in 2021/22 infographic
This infographic provides information on the number of Advanced services provided by community pharmacy teams in England during 2021/22.
Archived Advanced services
Community Pharmacist Consultation Service (CPCS) – This service ended on 30th January 2024. From 31st January 2024, the service was incorporated into the Pharmacy First service.
C-19 Lateral Flow Device Distribution Service – this service was decommissioned on 31st March 2022
Hepatitis C Testing Service – this service was decommissioned on 1st April 2023
Medicines Use Reviews (MURs) – this service was decommissioned on 31st March 2021
Pandemic Delivery Service (PDS) – this service was decommissioned on 31st March 2022